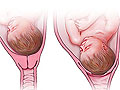
Topic Overview
Is this topic for you?
This topic provides basic information about normal labour and delivery. If you need information on pregnancy, other types of childbirth, or the first 6 weeks after childbirth (postpartum), see:
What is labour and delivery?
At the end of the third trimester of pregnancy, your body will begin to show signs that it is time for your baby to be born. The process that leads to the birth of your baby is called labour and delivery. Every labour and delivery includes certain stages, but each birth is unique. Even if you have had a baby before, the next time will be different.
Giving birth to a baby is hard work. It can also be scary, thrilling, and unpredictable. Learning all you can ahead of time will help you be ready when your time comes.
What are the stages of labour?
There are four stages of labour. The first stage includes early labour and active labour. The second stage lasts through the birth, with the baby travelling down and out of the birth canal. The third stage is after the birth, when the placenta is delivered. The fourth stage is the first few hours after the birth.
Stage one. The muscles of the uterus start to tighten (contract) and then relax. These contractions help to thin (efface) and open (dilate) the cervix so the baby can pass through the birth canal.
Stage one has three phases:
- Early. Early contractions are usually irregular, and they usually last less than a minute. The early phase of labour can be uncomfortable and may last from a few hours to days.
- Active. Contractions become strong and regular and last about a minute. This is the time to go to the hospital or birthing centre. The pain of contractions may be moderate or intense.
- Transition. The cervix will open completely. If there are no problems, the baby should be in position to be born.
Stage two. The cervix is dilated completely and the baby is born.
Stage three. This stage occurs after the baby is born. You have contractions until the placenta is delivered.
Stage four. This is the first few hours after the birth.
How can you manage pain?
Having a support person, trying different positions, or using breathing exercises may help you cope with labour pain. You also can listen to music or use imagery to distract you and help you relax. Some women labour in water or take a shower.
Many women ask for pain medicine, such as an epidural injection, which partially or fully numbs the lower body. Even if you plan to not use pain medicine (natural childbirth), it can be comforting to know that you can get pain relief if you want it.
How can you prepare for labour and delivery?
Getting regular exercise during pregnancy will help you handle the physical demands of labour and delivery. Try adding Kegel exercises to your daily routine. They strengthen your pelvic floor muscles. This helps prevent a long period of pushing during labour.
In your sixth or seventh month of pregnancy, consider taking a childbirth education class with your partner or support person. It can teach you ways to relax and the best ways for your support person to help you.
There are many decisions to make about labour and delivery. Before your last weeks of pregnancy, be sure to talk to your doctor or midwife about your birthing options and what you prefer.
You can write down all of your preferences as a birth plan. This gives you a chance to state how you would most like things to be handled. Just keep in mind that it is not possible to predict exactly what will happen during labour and delivery.
What can you expect right after childbirth?
Now you get to hold and look at your baby for the first time. You may feel excited, tired, and amazed all at the same time.
If you plan to breastfeed, you may start soon after birth. Don't be surprised if you have some trouble at first. Breastfeeding is something you and your baby have to learn together. You will get better with practice. If you need help getting started, ask a nurse or breastfeeding specialist (lactation consultant).
In the hours after delivery, you may feel sore and need help going to the bathroom. You may have sharp, painful contractions for several days as your uterus shrinks in size.
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
Planning for Birth
Consider a birth plan
During your prenatal visits, talk with your doctor about your labour and delivery options. You may want to write them down as a birth plan. It's an ideal picture of what you would like to happen.
But try to be flexible. No labour and delivery can be predicted or planned. So give yourself permission to change your mind at any time. And be prepared for your childbirth to be different from what you planned. If an emergency arises, your doctor has a responsibility to ensure both your safety and your baby's safety. You may still share in decisions, but your choices may be limited.
What to put in a birth plan
When you are writing your birth plan, think about:
- Who will deliver your baby.
- Where you want to have your baby. Most women choose to work with a doctor and have their baby delivered in a hospital. Women at low risk for problems may choose to work with a midwife or have their baby at a birth centre.
- Who you want to be with you. You may want to have family and friends around you or only the baby's other parent or another support person, such as a doula.
- Comfort measures you want to try. Breathing techniques, labouring in water, trying different positions, and having one-on-one support may help you manage pain.
- Your preferences for medical treatments. Consider what type of pain medicine you would prefer, even if you don't think you'll need it. Just keep in mind that you may not always get to choose.
- How your baby will be cared for after delivery. This might include having your baby stay in the room with you rather than going to the nursery, delaying some tests and procedures, and getting help with starting to breastfeed.
This is also a good time to decide whether you'll attend (if you haven't already) a childbirth education class, starting in your 6th or 7th month of pregnancy.
To help you get started on writing a birth plan, fill out the My Birth Plan form . Take it to your next appointment to discuss your wishes with your doctor or midwife.
What to expect at the hospital
You may feel more calm and prepared for labour if you know what is likely to happen when you get to the hospital.
Most hospitals and birthing centres have birthing rooms where women can labour, deliver, and recover. Providing that you have an uncomplicated birth, you can probably be in the same birthing room for your entire stay. If your delivery becomes complicated, you can be quickly moved to a delivery room equipped to handle the problem.
If you arrive at the hospital or birthing centre in early labour that is progressing quickly, you can expect some or all of the following:
- Your blood pressure, pulse, and temperature will be checked.
- You will be asked about the timing and strength of your contractions and whether your water has broken (your membranes have ruptured).
- Electronic fetal heart monitoring will be used to record the fetal heart rate as you have contractions. Fetal heart rate shows whether the baby is doing well or is in trouble.
- You will have sterile vaginal examinations to check whether your cervix is thinning and opening (effacing and dilating).
- You may have an intravenous (IV) needle inserted, in case you need extra fluids or medicine later on.
- You may be encouraged to walk. Walking helps many women feel more comfortable during early labour.
Newborn care decisions
Before your baby is born, plan ahead about:
- Keeping your baby with you for at least 1 hour after birth, for bonding. (Many hospitals allow rooming-in, with no mother-baby separation during the entire hospital stay.)
- Preventing breastfeeding problems. You can plan ahead for breastfeeding support in case you need it. Check around for a lactation consultant. Some hospitals have them in-house. You can also make sure that hospital staff knows not to give your baby supplemental formula, unless there is a medical need.
- Delaying certain procedures—such as a vitamin K injection, a heel prick for a blood test, and the use of eye medicines—so that you have more time to bond with your baby in the hours after birth.
- Whether and when you'd like visitors, including children in your family.
- Whether to bank your baby's umbilical cord blood after the birth. (This requires advance planning early in your pregnancy.)
Signs of Labour
No one can predict when labour will start. One woman can have all the signs that her body is ready to deliver, yet she may not have the baby for weeks. Another woman may have no advance signs before she goes into active labour. First-time deliveries are harder to predict.
Signs that labour may start soon
Late in your pregnancy, your doctor or midwife will tell you what to do when you think you are in labour. Early labour can be different for every woman. At first, your contractions may not be regular, and they may happen only now and then.
You may have signs that early labour is not far off.
- The baby may settle into your pelvis. Although this is called dropping, or lightening, you may not feel it.
- Your cervix may begin to thin and open (cervical effacement and dilatation). Your doctor checks for this during your prenatal examinations.
- Braxton Hicks contractions may become more frequent and stronger, and perhaps a little painful. You may also feel cramping in the groin or rectum or an ongoing ache low in your back.
- Your amniotic sac may break (rupture of the membranes). In most cases, rupture of the membranes occurs after labour has already started. In some women, this happens before labour starts. Call your doctor right away or go to the hospital if you think your membranes have ruptured.
The key to knowing when you're in labour is that the contractions start to get longer, stronger, and closer together. You will feel them even when you change positions and are walking or moving around. After a while, it will become hard for you to talk during a contraction. You may have to stop to focus on your breathing.
When to call a doctor
Many women stay at home during early labour. During this time, it's important to know when to call your doctor or midwife.
You or someone else should call 9-1-1 or other emergency services immediately if you think you may need emergency care. For example, call if you:
- Have severe vaginal bleeding.
- Have severe pain in your belly or pelvis.
Call your doctor now or go to your hospital's labour and delivery unit immediately if you:
- Have any vaginal bleeding.
- Have had regular contractions for an hour. This means about 4 or more in 20 minutes, or about 8 or more in 1 hour, even after you have had a glass of water and are resting.
- Have a sudden release of fluid from your vagina. It is possible to mistake a leak of amniotic fluid for a problem with bladder control.
- Have low back pain or pelvic pressure that does not go away.
- Have noticed that your baby has stopped moving or is moving much less than normal. See kick counts for information on how to check your baby's activity.
Managing Pain
You can choose from several types of pain relief for childbirth. These include medicine or breathing techniques, as well as comfort measures. You also can use a combination of these choices.
Comfort measures
There are many ways to reduce the stresses of labour and delivery. "Natural" childbirth techniques (without medicine) may help reduce pain and help you feel a sense of control during labour. Consider:
- Continuous labour support. Having a support person with you from early labour until after childbirth has a proven, positive effect on childbirth.footnote 1
- Distraction. During early labour, you can walk, play cards, watch TV, take a shower, or listen to music to help take your mind off your contractions.
- Massage. Massage of the shoulders and lower back during contractions may ease your pain. Strong massage of the back muscles (counterpressure) during contractions may help relieve the pain of back labour. Tell your labour coach exactly where to push and how hard to push.
- Imagery. Imagery is using your imagination to decrease your pain. For instance, to help manage pain, visualize contractions as waves rolling over you. Picture a peaceful place, such as a beach or mountain stream, to help you relax between contractions.
- Changing positions during labour. Walking, kneeling, or sitting on a big rubber ball (birth ball) are good options. For more information see Labour Positions.
- Focused breathing techniques. Breathing in a rhythm can distract you from pain. Childbirth education classes will teach you different methods of focused breathing.
- Labouring in water. Soaking in warm water may help with pain, stress, and sometimes slow, difficult labour.footnote 2
Other techniques without medicine
Other techniques that don't use medicine to control pain include:
- Hypnosis. This is a low-risk way of managing labour pain and anxiety that works for some women.footnote 3
- Acupuncture. Small studies suggest that acupuncture is a low-risk, effective way of managing labour pain for some women.footnote 3
Pain relief with medicine
Your options for pain relief with medicine may include:
- Opioids (narcotics), which are used to reduce anxiety and partially relieve pain. An opioid is less likely than epidural anesthesia to lead to an assisted (forceps or vacuum) delivery.footnote 4 But an opioid is usually not used when you are close to delivery, because it can affect a newborn's breathing.
- Epidural anesthesia, which is an ongoing injection of pain medicine into the epidural space around the spinal cord. This partially or fully numbs the lower body.
- Pudendal and paracervical blocks. These are injections of pain medicine into the pelvic area to reduce labour pain. Pudendal is one of the safest forms of anesthesia for numbing the area where the baby will come out. It can be helpful with fast labour when a little pain medicine is needed close to delivery.
Some pain-relief medicines aren't the type that you would request during labour. They are used as part of another procedure or for an emergency delivery. But it's a good idea to know about them.
- Local anesthesia is the injection of numbing pain medicine into the skin. This is done before inserting an epidural or before making an incision (episiotomy) that widens the vaginal opening for the birth.
- Spinal block is an injection of pain medicine into the spinal fluid. It quickly and fully numbs the pelvic area for assisted births, such as a forceps or caesarean delivery.
- General anesthesia is the use of inhaled or intravenous (IV) medicine, which makes you unconscious. It has more risks, yet it takes effect much faster than epidural or spinal anesthesia. So general anesthesia is usually only used for some emergency C-sections that require a rapid delivery.
Types of Delivery
Most babies are born in a vaginal delivery. But in some cases, other types of delivery occur by choice or because of an emergency.
Vaginal birth
During labour, the uterus contracts regularly to thin and open (efface and dilate) the cervix and push the baby out through the birth canal. It can take many hours or days for the cervix to open all the way so you can begin pushing.
Caesarean birth
A caesarean section is the delivery of a baby through a cut (incision) in the mother's belly and uterus. It is often called a C-section. In most cases, a woman can be awake during the birth and be with her newborn soon afterward.
A C-section may be planned or unplanned. In most cases, doctors do caesarean sections because of problems that arise during labour. For more information, see the topic Caesarean Section.
Vaginal birth after caesarean
In the past, a woman who had one C-section delivery had to have all of her other babies by C-section. But depending on the reason for your first C-section and the type of incision that was made, you may be able to deliver your next baby vaginally.
For more information, see the topic Vaginal Birth After Caesarean (VBAC).
Stages of Labour
The process of having a baby occurs in several stages over many hours or even a few days—from early labour through delivering the baby and the placenta. During labour, contractions in your uterus open your cervix and move the baby into position to be born.
Stage one: Early, active, and transition
Early labour
Early labour is often the longest part of the birthing process, sometimes lasting 2 to 3 days. Uterine contractions:
- Are mild to moderate (you can talk while they are happening) and last about 30 to 45 seconds.
- May be irregular (5 to 20 minutes apart) and may even stop for a while.
- Open (dilate) the cervix to about 3 cm (1 in.). First-time mothers can have many hours of early labour without the cervix dilating.
It's common for women to go to the hospital during early labour and be sent home again until they are in active labour or until their "water" breaks (rupture of the membranes). This phase of labour can be long and uncomfortable.
Active labour
The active stage of labour starts when the cervix is about 3 cm (1.2 in.) to 4 cm (1.6 in.) dilated. This stage is complete when the cervix is fully effaced and dilated and the baby is ready to be pushed out.
Compared with early labour, the contractions during active labour are more intense and more frequent (every 2 to 3 minutes) and longer-lasting (50 to 70 seconds). Now is the time to be at or go to the hospital or birthing centre. If your amniotic sac hasn't broken before this, it may now.
As your contractions get stronger, you may:
- Feel restless or excited.
- Find it hard to stand up.
- Not be allowed to eat or drink. Some hospitals let you drink clear liquids. Others may only allow you to suck on ice chips or hard candy.
- Want to start using breathing techniques or other ways to control pain and anxiety.
- Feel the need to shift positions often. This is good for you, because it improves your circulation.
- Want pain medicine, such as epidural anesthesia.
- Be given intravenous (IV) fluids.
To learn more about pain medicine, see Managing Pain.
Transition
The end of active labour is called the transition phase. As the baby moves down, your contractions become more intense and longer and come even closer together.
When you reach transition, your delivery isn't far off. During transition, you will be self-absorbed, concentrating on what your body is doing. You may be annoyed or distracted by others' attempts to help you but still feel you need them nearby as a support. You may feel increasingly anxious, nauseated, exhausted, irritable, or frightened.
A mother in first-time labour will take up to 3 hours in transition, and a mother who has vaginally delivered before will usually take no more than an hour. Some women have a very short, if intense, transition phase.
Stage two: The baby is born
The second stage is the actual birth, when the baby is pushed out by the contractions. This pushing stage can be as short as a few minutes or as long as several hours. You are more likely to have a fast labour if you have given birth before. During the second stage:
- Uterine contractions will feel different. Though they are usually regular, they may slow down to every 2 to 5 minutes, lasting 60 to 90 seconds. If your labour stalls, changing positions may help. If not, your doctor may recommend using medicine to stimulate (augment) contractions.
- You may have a strong urge to push or bear down with each contraction.
- You may need to change position several times to find the right birthing position for you.
- You can have a mirror positioned so you can watch your baby as the head comes through the vagina (called crowning).
- When the baby's head crowns, you will feel a burning pain. If this is happening quickly, your doctor may advise you not to push every time, which may give the perineum, which is the area between the vulva and the anus, a chance to stretch without tearing.
Your medical staff will be ready to handle anything unexpected. This is a time when your doctor or midwife will be deciding what is best for you and your baby.
Stage three: The placenta is delivered
After your baby is born, your body still has some work to do. This is the third stage of labour, when the placenta is delivered. You will still have contractions. These contractions make the placenta separate from the inside of the uterus, and they push the placenta out. Your medical staff will help you with this. They will also watch for any problems, such as heavy bleeding, especially if you have had it before.
You may be given some medicine to help the uterus contract firmly. Oxytocin may be given as a shot or in a vein (intravenously) after the placenta is delivered. Oxytocin is given to make your uterus shrink and bleed less. (This is the same medicine that is sometimes used to make contractions more regular and frequent during labour.) Breastfeeding right away can also help the uterus shrink and bleed less.
The third stage can be as quick as 5 minutes. With a preterm birth, it tends to take longer. But in most cases, the placenta is delivered within 30 minutes. If the placenta doesn't fully detach, your doctor or midwife will probably reach inside the uterus to remove by hand what is left inside. Your contractions will continue until after the placenta is delivered, so you may have to concentrate and breathe until this uncomfortable process is complete.
Stage four: After childbirth
It is normal to feel excited, tired, and amazed all at the same time after delivery. You may feel a great sense of calm, peace, and relief as you hold, look at, and talk to your baby. During this stage you will be watched closely for any problems.
Breastfeeding
During the first hour after the birth, you can also expect to start breastfeeding, if you plan to breastfeed.
If you breastfeed, don't be surprised if you and your baby have some trouble doing it at first. Breastfeeding is a learned technique, so you will get better at it with practice. You may have a breastfeeding specialist (lactation consultant) in the hospital to help you get started.
For information about getting a good start with breastfeeding and preventing problems, see:
Your first hours of recovery
You may have shaking chills right after delivery. This is a common reaction in the hours after delivery. A warm blanket may help you feel more comfortable.
During the first hours after the birth, your health professional or a nurse will:
- Massage your uterus by rubbing your lower abdomen about every 15 minutes. Later, you will be taught to massage your own uterus. This helps it tighten (contract) and stop bleeding.
- Check your bladder to make sure it isn't full. A full bladder puts pressure on your uterus, which interferes with contractions. You will be asked to try to urinate, which may be hard because of pain and swelling. If you can't urinate, a tube (catheter) can be used to empty your bladder.
- Check your blood pressure frequently.
- Repair the area between your vagina and anus (perineum) if it tore or if you had an incision (episiotomy).
- Remove the small tube in your back if you had epidural anesthesia. If you plan to have a tubal ligation surgery to prevent future pregnancy, the catheter will be left in.
You may also have:
-
Certain immunizations.
- Tetanus, diphtheria, and pertussis (Tdap). If you need a booster for these immunizations, you may get it soon after you have your baby, before you go home from the hospital.
- Measles, mumps, and rubella (MMR). If you are not immune to rubella or measles, your doctor may recommend that you have the MMR vaccine after childbirth.
- An Rh immunoglobulin shot (such as WinRho). If you have Rh-negative blood, you may get a shot of Rh immunoglobulin after delivery if your newborn is Rh-positive. For more information see the topic Rh Sensitization During Pregnancy.
Labour Positions
In most cases, you don't have to lie in bed the whole time you're in labour. (If you have an epidural or have certain health problems, you may have to stay in bed.) You can choose whichever position feels most comfortable. You may want to walk, sit on a big rubber ball, or kneel. The position that feels best for you may change as you move through labour:
Moving around and changing positions during labour may help you feel more comfortable and might help reduce the length of labour.footnote 5
Birthing positions
Birthing positions for pushing include squatting, reclining, or using a birthing chair, stool, or bed. You may find that certain positions are more comfortable than others during the pushing stage. Speak to your doctor or midwife about different birthing positions before your labour begins.
- Kneeling, getting down on your hands and knees, or leaning onto a birthing ball may help to take pressure off your back. This position might also help with back labour.
- Squatting may help you push more effectively.
- Lying on your back in a semi-reclining position with your legs supported by foot supports. While pushing, your doctor or midwife may have you grab behind your knees and pull up.
- Lying on your side is helpful if you are tired of lying on your back.
- Some birthing centres use a birthing stool or chair during the pushing stage. A birthing chair may help you feel more comfortable.
Medical Procedures
In some cases, a woman may need medical help to give birth. For instance, labour may stall, or the baby may need help to get through the birth canal. Sometimes what starts as a routine vaginal birth may end in a caesarean delivery to make sure the mom and baby are safe.
Procedures done during labour
Fetal heart monitoring and vaginal examinations are standard practice during labour, but other procedures are used as needed.
- It's helpful to know about the types of fetal monitoring you may have. Monitoring may be either continuous for a high-risk delivery, or periodic to check for signs that the baby may be in distress.
- You will have sterile vaginal examinations to check whether your cervix is thinning and opening (effacing and dilating).
- Labour induction and augmentation includes a simple "sweeping of the membranes" just inside of the cervix, rupturing the amniotic sac, using medicine to soften (ripen) the cervix, and using medicine to stimulate contractions. This may be needed if your baby is overdue (post-term pregnancy).
- Antibiotics if you tested positive for group B strep during your pregnancy.
Procedures to help with delivery
Sometimes your doctor may need to use different procedures to help deliver the baby.
- Forceps delivery or vacuum extraction is used to assist a vaginal delivery. This may be needed when labour is stalled at the pushing stage or when the baby shows signs of distress at the pushing stage and needs to be delivered quickly.
- Episiotomy widens the perineum with an incision. This is sometimes used to deliver the baby's head more quickly, when there are signs of distress.
- The need for a caesarean birth during labour is mainly based on the baby's and mother's conditions. For more information, see the topic Caesarean Section.
Related Information
References
Citations
- Hodnett ED, et al. (2012). Continuous support for women during childbirth. Cochrane Database of Systematic Reviews (10).
- Cluett ER, Burns E (2009). Immersion in water in labour and birth. Cochrane Database of Systematic Reviews (2).
- Smith CA, et al. (2006). Complementary and alternative therapies for pain management in labour. Cochrane Database of Systematic Reviews (4).
- Cunningham FG, et al. (2010). Forceps delivery and vacuum extraction. In Williams Obstetrics, 23rd ed., pp. 511–526. New York: McGraw-Hill.
- Lawrence A, et al. (2009). Maternal positions and mobility during first stage labour. Cochrane Database of Systematic Reviews (2).
Credits
Adaptation Date: 10/2/2023
Adapted By: HealthLink BC
Adaptation Reviewed By: HealthLink BC
Adaptation Date: 10/2/2023
Adapted By: HealthLink BC
Adaptation Reviewed By: HealthLink BC